Chapter 1
Trend one: Humans at the center
How will you utilize technologies to make health care even more human?
At present, patient-consumers have to fit into a very disparate and inconvenient health infrastructure. The current model is siloed, provider-driven and supply-oriented. The future model will be connected and driven by customer demand.
To deliver the personalized, seamless and informed experience that patient-consumers increasingly want and expect, companies will have to collaborate to rebuild the health care ecosystem around the patient. This patient-centered model of care will need data to be aggregated and shared to more fully understand and respond to patient-consumers’ needs and desires. Health care needs to come to the patient rather than the patient spending their time and energy navigating the system.
Technologies are already helping to connect patients and deliver services. Telehealth is the obvious example in 2020, with Teladoc’s US$18.5b acquisition of Livongo signaling the rapid maturing of the remote care industry. But beyond this headline-making deal, leveraging technology to make the experience faster, more frictionless and more effective is advancing in multiple areas. And it’s not only health providers and payors who are now focusing on the Health Experience; some biopharmas, too, already understand they have to go beyond selling the product to engaging with the patient, understanding the patient’s journey and delivering to them not just better care but a better care experience. Some examples:
- AstraZeneca launched AMAZE, a cloud-based platform to manage chronic disease (for example in the respiratory, cardiac and renal areas) in March 2020. The company envisages all patients in the future taking home two prescriptions: one for the medicine, the other for the digital tools enabling the patient and clinician to monitor the response to the medicine after the patient is discharged and to change the care plan as needed.
- Roche is streamlining clinical trials to make them easier to participate in, both for the patients and the clinicians. One example is the Prospective Clinico-Genomic Study, which is a feasibility study that is run together by Roche-owned Flatiron Health, Foundation Medicine and Genentech. This study uses liquid biopsy and remote monitoring to capture many different data streams without the patient having to undergo regular invasive tests in the hospital. By gathering these data the company is trying to understand the patient’s journey and build a highly personalized treatment plan to improve it.
- Novartis and Biofourmis have developed a platform that tracks the condition of heart failure patients. Patients leave the hospital with Novartis’ heart failure treatment Entresto and with Bioufourmis’ Everion sensor, which measures 22 biometrics in real time to constantly monitor the patient’s condition and allow clinicians to respond rapidly if needed.
- Pear Therapeutics and etectRx signed a January 2021 deal to integrate Pear’s innovations (pioneering digital therapeutics for drug abuse and insomnia) with smart pills (which include an ingestible wireless sensor to track adherence). The combined platform will offer richer ways to engage and assist patients, and the two companies intend to approach pharma collaborators with the aim of incorporating this technology into clinical trial programs.
- Color Genomics, which originally focused on cancer diagnostics, is now accelerating COVID-19 testing across the US. The unique value the company offers goes beyond its actual test to its scalable and flexible “infrastructure” now reaching patients wherever they are – in schools and workplaces as well as in hospitals and clinics. The company has road mapped the journey the broader industry needs to take by moving beyond the product to take on the challenges of increasing access, reducing friction and improving experiences.
The future health care network now emerging is built on rapid, 5G-enabled connections between sensors inside our bodies, on our skin and in the environment around us and AI algorithms that interrogate these data and generate detailed insights. The rich, continuous data and insights generated by this network will be critical to putting humans at the center and delivering the integrated, personalized solutions that empower the individual patient-consumer.
Delivering these solutions will mean different things for different companies, depending on the business model they choose:
- Breakthrough innovators will need to deploy sensors that can capture individual genetic and phenotypic information, so they can offer high precision, personalized therapies and in some cases personalized medicines that are potentially curative. Cell and gene therapies are one area where this approach is becoming a reality.
- Disease managers will need to focus on offering the right personalized mix of products, services and information. These offerings will be built on sensors that can help clinicians monitor and manage patients’ disease progression to achieve good health. This will not just mean, for example, delivering the patient a product to treat their heart disease; it will mean building a more complete understanding of the patient’s disease status (not just heart disease, but all comorbidities affecting that patient), and monitoring and managing their status continuously.
- Efficient producers will need agile operations built around sensors that can capture data that enables them to respond to customer demands and other market signals rapidly and at minimum marginal cost, and ensure steady affordable supplies of commodity drugs and devices to market.
- Lifestyle managers will depend on sensors that can capture individual consumer preferences and lifestyle choices, allowing them to offer the right personalized mix of consumer health products, nudges, nutrition coaching and other assistance.
To put humans at the center, companies must:
- Partner with or acquire companies to access new capabilities in user-centered design, behavioral science and services.
- Build or buy expertise in, on and around the body sensors analytics, AI and machine learning algorithms and interoperable system integration.
- Target development of better health solutions that integrate drugs with convenient-to-use devices and diagnostics.
Chapter 2
Trend two: Supply chain
How will your operating model adapt to deliver products and services anywhere?
Companies must deliver value from services, not just products. Today’s linear supply chains deliver high service levels and meet regulators’ demands for compliance, but they are not built for speed or agility. The industry’s supply chains proved resilient during the pandemic, but companies also learned the limitations of their globalized supply chains when dealing with significant disruptions in cross-border trade.
In particular, today’s health sciences and wellness supply chains lack end-to-end visibility. Companies do not have transparency into their supplier or contract manufacturing base. It’s currently difficult if not impossible for companies to share data with network partners given the lack of connectivity in the digital technologies on which their supply base depends. Personalized care models require a different level of supply chain transparency and integration.
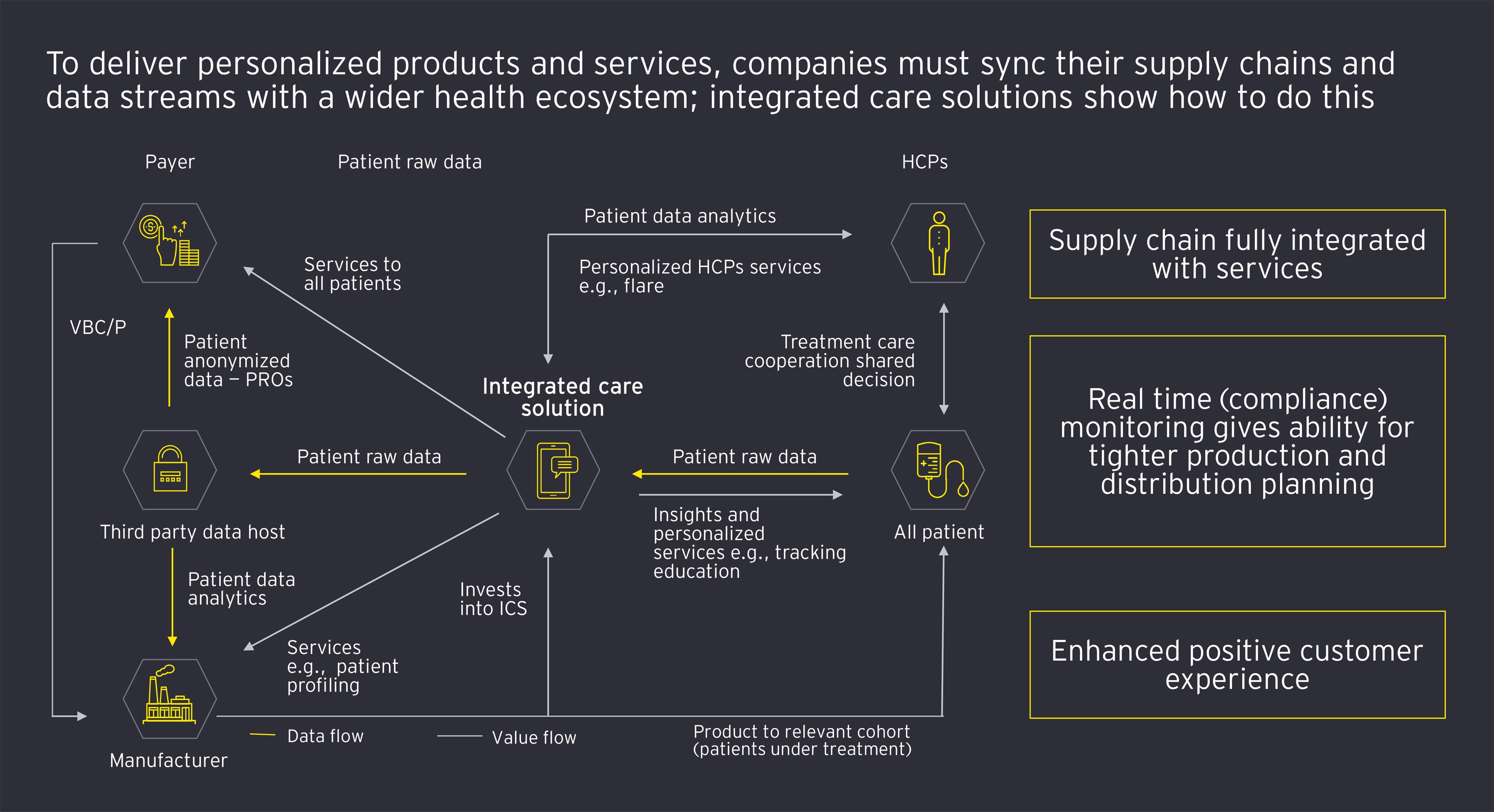
Personalized care means different things for different business models:
- For breakthrough innovators, a personalized supply chain could mean a supply chain that delivers an individualized product, for example, an autologous cell therapy, in which the therapy is manufactured from the patient’s own cells.
- For disease managers, a personalized supply chain will mean a supply chain that can deliver the right products and the right services that wrap around these products and make patients, for example, more compliant. This can include digital tools that remind the patient to take their medicine and check to confirm they take it correctly or sensors that monitor their health to help ensure chronic conditions are under control.
- For efficient producers, the challenge is to develop supply chains that are extremely agile, flexible and robust; able to operate at very high utilization levels while predicting demand levels, e.g., by anticipating tender wins.
- For lifestyle managers, the supply chain will make use of predictive analytics that can proactively manage and influence consumer demand, anticipating what individuals want and offering them solutions.
These personalized future supply chains will need to draw raw material such as cells and/or individualized data from patients even as they deliver products and services to patients, to enable further real-time refinement of care.
To deliver personalized care companies will also need to build flexible partnerships to connect faster across increasingly complex networks, interfacing data as necessary with hospitals, physicians, manufacturers, caregivers and diagnostic labs. These networks will also likely include partnerships with new market entrants to address supply gaps.
To deliver personalized supply chains, companies must:
- Prioritize end-to-end supply chain visibility, from the patient all the way to the supplier networks, to strengthen risk management and resilience and allow real-time use of market signals and rapid decision-making.
- Develop the ability to rapidly build and integrate new supply chains and entire manufacturing systems in parallel with clinical development of innovative products.
- Develop product- and process-based partnerships that enable flexible, fast connections across a variety of supply chain networks.
Chapter 3
Trend three: Demonstrating measurable outcomes
How will you bridge trust gaps and build mutual value together?
Worldwide, health care takes a growing proportion of GDP. As treatments become more personalized, the corresponding complexity will – at least in the short term – create increasing cost pressures that make the adoption of new outcomes-based payment models more urgent. Although fee-for-service remains the primary reimbursement model, companies that want to be rewarded for their personalized innovations will need to show how these products and services offer greater value to specific health stakeholders and the ecosystem overall.
While payers, governments, care providers and consumers all seek better health outcomes, the definition of value and their respective stakes are not always aligned. Innovative contracts can play an important role in reinforcing the alignment of value. Consider the adoption of new pharmaceutical products: clinical trials will ascertain a product’s medical efficacy and expected outcomes; health care systems will reimburse for products that deliver demonstrable health care benefits.
But until those better outcomes are demonstrated in the real world, providers will be reluctant to prescribe and payers reluctant to reimburse, and fewer patients will get the chance to experience the benefits. A contract that connects a product’s reimbursement to its real-world performance shares the risk between providers and pharmaceutical companies and enables faster market access.

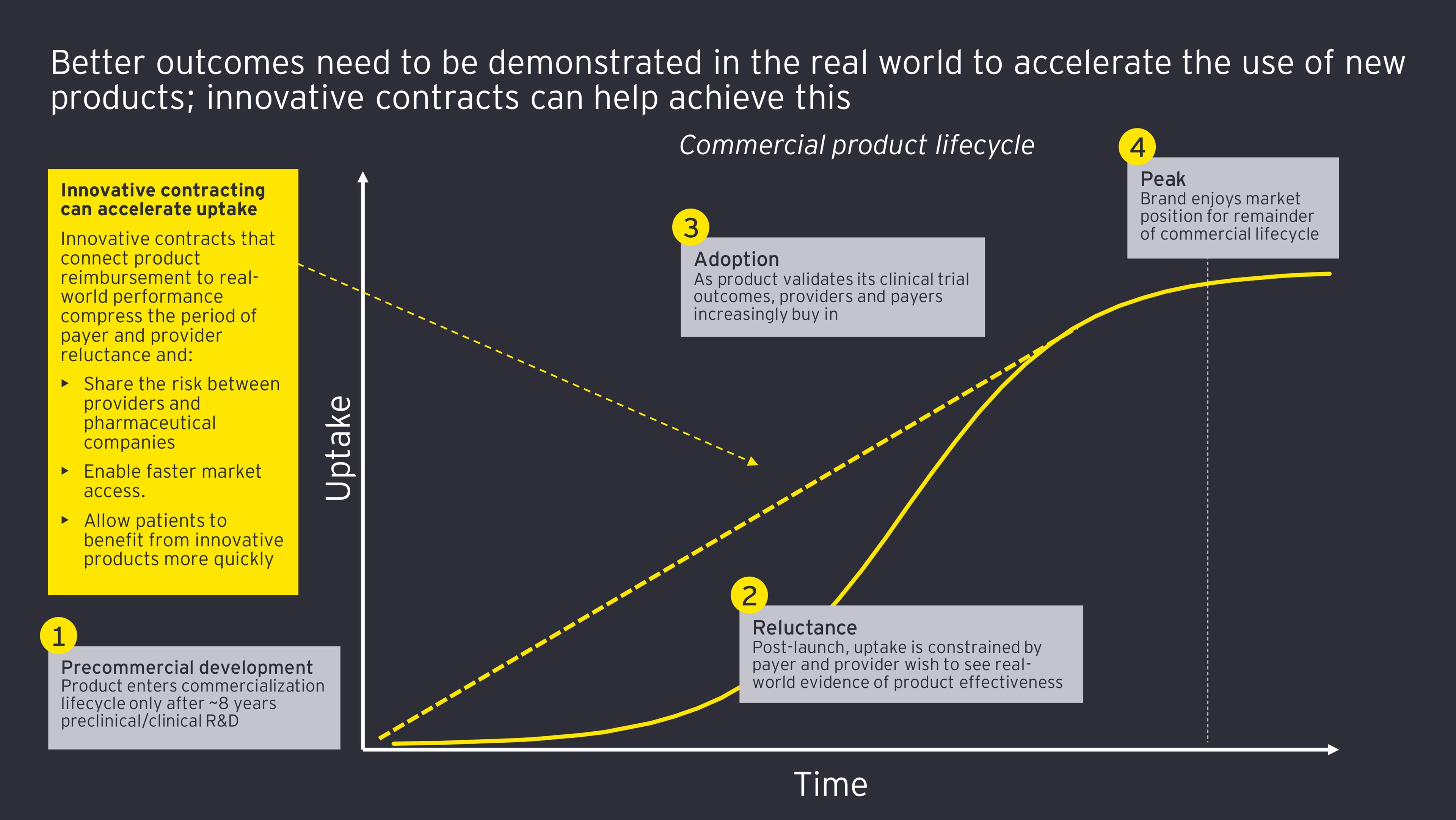
In the past, innovative contracts have proved complicated to implement, costly to administer and convoluted to scale across different payers and geographies. Now, companies have the opportunity to resolve these problems; for example, through the use of platform technologies that allow data to be captured, shared and validated by different parties and thus reduce key barriers linked to administration and wide-spread adoption.
Agreeing on the data that actually demonstrate value is a more challenging issue. Stakeholders, especially payers and life sciences companies, need to agree on which outcomes are meaningful to them and the time frame for measurement. Increasingly, clinical data alone will not be sufficient to make these value assessments: real-world data linked to the efficiency and location of care delivery capture important potential cost-savings for hospitals and health systems. And of equal importance, patients’ increased quality of life and improved ability to adhere to medications – their experience – can be better measured and served by innovative contract approaches.
Cost of treating diseases is rising
US$475,000is how much list prices of new cell and gene therapies have risen.
Ultimately, the data that will be of highest value will depend on a number of factors including the severity of disease and the ability to prevent, manage or treat it. For life sciences companies, it will also depend on which stakeholders are demanding the value (is it the consumer or the health system?) and how is that value being created (is it innovative products and services or an exquisite understanding of the customer)? In other words, deciding which outcomes data to prioritize should be directly informed by a company’s given business model.
- Because they create value through highly innovative products and services, breakthrough innovators should prioritize the collection of personalized clinical data, including genomic or other companion diagnostics.
- Efficient producers deliver the most value through their cost-effective delivery of treatments and services. As such, they need to capture data demonstrating they reduce the cost of care at the population level.
- For disease managers and lifestyle managers, non-clinical measures of outcomes will be critical to measure. Companies working in these business models must manage the holistic patient experience and access data that measure more humanistic types of value. For example, quality of life: an individual’s ability to remain in the workforce, live independently and avoid disease flare ups or side-effects are all meaningful outcomes to individuals living with chronic inflammatory or neurodegenerative conditions. Because these diseases affect significant numbers of people, the ability of medicines to reduce their number of disability-adjusted life years (a metric economists use to quantify the loss in productivity associated with ill health) should also be of interest to the employers and institutional health care systems that help pay for this care.
In order to demonstrate better measurable outcomes, accelerate the use of innovative contracts and position themselves to outperform, companies must:
- Proactively model how the use of products and services generate cost-savings for health systems and productivity gains for employers and individuals.
- Collaborate with consumer, technology and other organizations to develop digital tools and services that are easy to use and increase adherence to treatment and validate its effectiveness.
- Work with regulators to better use real-world data in product approvals and reimbursement decisions.
Chapter 4
Trend four: Data
Who will you partner with to access the data you don’t own, but need?
The health industry generates unprecedented volumes of data every year that sit in siloes, and because of this, the true and extended value that can be mined from it is very challenging to extract. Technical difficulties, regulatory reluctance and “ownership” issues make it difficult to break down these siloes. However, the greater challenge is often the attitude of companies themselves: companies too often view data only as an asset to protect. They are reluctant to increasing the ease with which their data can be transferred across systems fearing it might give competitors access to what they consider potential but unexplored and the possible unregistered IP that may lie within its analysis.
Health care companies’ data generation is growing at nearly 900% this year.
50 terabyteswas the average data generated in 2020 by every person on the earth
But with health data growing at an exponential rate, the reality is that no company can or should own more than a negligible fraction of the total volume. Nor should they want to: what matters is not the volume of raw data a company has on its servers (whether structured or unstructured), but the data it can access, interrogate and leverage. Owning data is a cost but accessing and interrogating data will generate insights and value to the health system. The value lies not in monetizing proprietary data assets, but in asking the right questions and connecting and combining disparate data streams to answer them.
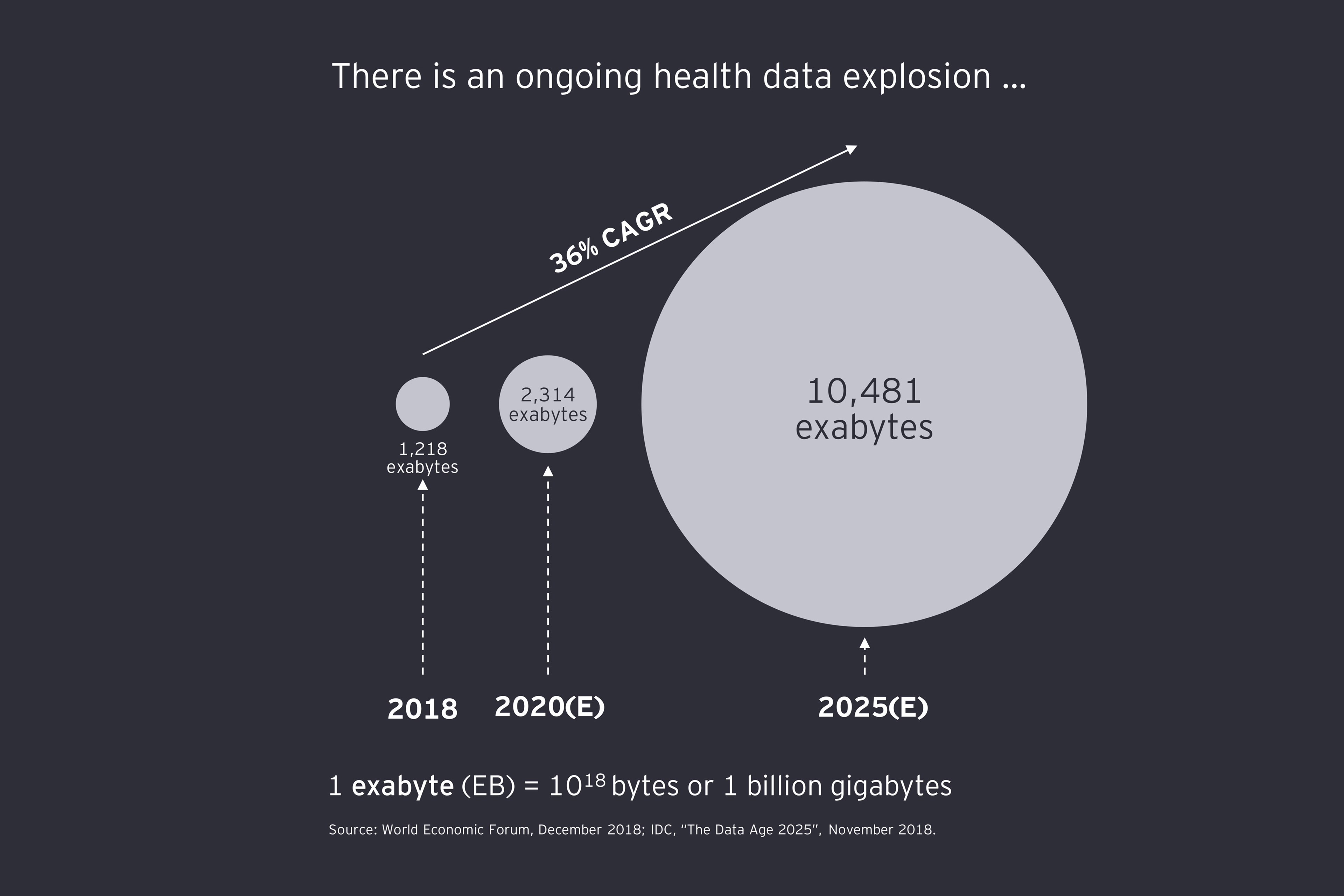
To refuse to share or grant access to data therefore significantly slows the rate of meaningful progress in health. In the long term, as health care technologies link up, a connected, flexible information architecture will emerge to enable a qualitatively better level of health data liquidity. This frictionless, “superfluid” data environment will hold unlimited potential to drive new insights that can transform health care. For now, however, companies must take a more limited and tactical approach to the challenge of data. The two key questions all companies must address are:
- How can a company access the data they need?
- Which data are the most important to their business model?
Companies are already exploring multiple approaches to access the rich, longitudinal patient-level data held within health systems. Health systems in turn can benefit from allowing companies to connect and combine datasets and share insights. For example, the UK NHS could generate an estimated £4.6b (roughly US$6.33b) through operational savings, enhanced patient outcomes and wider economic benefits if it allowed companies access to its 55 million patient records.1 While privacy and data security laws limit data sharing between health systems and life sciences companies, they can collaborate on workarounds such as “safe spaces” for data access, trusted research environments and arrangements with third-party data brokers.
With the advent of sensors and continuous data streams, these large longitudinal historic data sets may become less relevant and valuable to mine in the future. Dense and comprehensive seams of clinical and non-clinical data relevant to the patient-consumer – whether captured from sensors, social media, socioeconomic metrics or multiple other potential sources over a current discrete period in time – may prove to be more valuable. Ultimately, which data companies prioritize will depend on their business model approach:
- Breakthrough innovators should focus on genomic, phenotypic, biomarker and other data that can drive precision health, analyze and fine-tune patient response, and streamline clinical trials, by, for example, simulating control groups to predict outcomes.
- Disease managers need a range of personal clinical and non-clinical data to analyze complex chronic disease and select the right tools for personalized management, including the behavioral data that can help coach patients toward compliance and improved self-care.
- For efficient producers, the critical data are those that allow faster and more cost-effective decision-making at every point across the value chain, which helps with streamlining, automating and accelerating processes.
- Lifestyle managers need personalized data that allow them to proactively engage individuals about their health, predict consumer behavior and preferences and customize interactions.
To help ensure access to the data they need to drive clinical and commercial success, companies must:
- Develop trusted research environments, federated data system arrangements and other innovative solutions allowing vetted companies to access and use data.
- Work more closely with regulators and health stakeholders to establish norms for cybersecurity and other systemic standards that protect data integrity.
- Retrain or retain talent to develop proprietary algorithms and other data products that can accelerate R&D processes.
Chapter 5
Trend five: Sustainability
Does your business model give others confidence that your practices are sustainable and are focused on long-term value-generation?
Increasingly, consumers and investors will use a different formula to evaluate tomorrow’s health care brands, putting greater emphasis on their environmental sustainability and wider social impact. A survey of nearly 15,000 consumers conducted by EY professionals in February 2021 found that 45% of respondents believe that sustainability is more important than it was one year ago.
Larry Fink, Chairman and CEO of BlackRock, also emphasized this “sustainability premium” in his 2021 letter to CEOs. Based on BlackRock’s analysis, companies with better environmental, social and governance (ESG) profiles in the automotive, banking and energy industries outperformed their peers – and not just in the court of public opinion. As Fink eloquently reminded the business community, “The more your company can show its purpose in delivering value to its customers, its employees and its communities, the better able you will be to compete and deliver long-term, durable profits for shareholders.”2
As the demand to measure and report sustainability practices grows, it’s highly likely that access to capital will be more closely tied to ESG disclosures. Indeed, through the first 11 months of 2020, investors in mutual and exchange-traded funds invested nearly US$290b in sustainable assets, a 96% increase compared with 2019. Moreover, anecdotal evidence suggests biopharma and medtech companies are receiving better terms on debt because of their sustainability compliance.
To improve their sustainability agendas, life sciences and health companies must tackle a more fundamental challenge: identifying which specific metrics they should monitor and report in the first place. It may seem obvious that products and services that help people manage or treat disease have enormous social value. But in ESG terms, these offerings aren’t just an “S” issue. Environmental and economic issues matter, too. There is a clear linkage between worsening climate and poor health due to the increased incidence of chronic diseases such as asthma and diabesity. Companies developing treatments for these conditions therefore have a responsibility to keep a critical eye on their manufacturing sites and supply chains.
The issue is that there are dozens of sustainability metrics in use today. With no standard agreement on what “good” looks like, companies have been free to emphasize the metrics where they excel and minimize the rest. Such selective reporting creates investor skepticism and holds the industry back in another fundamental way: it’s impossible to make meaningful comparisons between companies’ sustainability agendas.
Based on a review of metrics developed by the Global Reporting Initiative, the Sustainability Accounting Standards Board and others, we believe it is time for companies to prioritize sector-specific metrics linked to four different dimensions. These dimensions directly reflect the social and environmental value of health offerings and can be categorized according to the following themes:
- Responsible innovation: A measure that reflects how new products and services address unmet disease needs and cure both common and neglected health conditions.
- Access and affordability: A measure that indicates the improvement in public health that results from making life-saving therapies and services widely available and reasonably priced.
- Trust and quality: Companies need to have a strong focus on the quality, safety and security of the therapies and services they provide, including complying with ethical promotional practices.
- Health impact on climate change: Because climate change has direct health implications, companies need to measure their carbon emissions, water and waste management protocols to limit the additional disease burden caused by their environmental and supply chain practices.
Within each one of these dimensions are a number of metrics worth tracking. Metrics linked to responsible innovation, for instance, could include: the number of products and services aimed at curing or modifying disease and the number of products in a company’s portfolio that address unmet medical needs. Measures of affordability and access, meanwhile, could include scores on the Access to Medicines Index, a recognized benchmark of how biopharma product value improves health outcomes and enables access to needy patients. As companies focus on the metrics that reflect their core value proposition, they should also prioritize measures based on their business models.
- Breakthrough innovators, for instance, are likely to create the most value by emphasizing responsible innovations – especially curative products that address unmet medical needs around the globe.
- Disease managers, meanwhile, create value by building closer relationships with the patients they keep healthy through the optimal management of their chronic conditions. Ensuring their offerings maintain compliance with current regulatory guidelines will be a critical need. This includes emerging standards linked to the privacy and security of medical data generated from the use of medical products and services.
- Efficient producers create value by keeping people economically productive. Making sure their medicines and services are affordable and accessible to the greatest number of people is of the highest importance.
- Lifestyle managers primarily focus on consumer offerings linked to wellbeing or pre-disease. As such, they should focus on metrics that show their commitment to broader environmental sustainability (for example, through demonstrating cleaner manufacturing and supply chain practices). EY survey data indicates that 72% of consumer respondents believe that companies’ behaviours are as important as the products they sell, meaning companies need to show that they share customers’ broader ethical values to secure market share in consumer health.
To demonstrate their commitment to sustainability, companies must:
- Establish a framework for measuring progress against sustainability goals linked to four themes: responsible innovation, access and affordability, trust and compliance and climate change.
- Prioritize metrics based on their specific business models. Developers of breakthrough innovations are most likely to create the most value by focusing on the development of curative medicines that address unmet medical needs, including future global infectious diseases.
- Monitor and communicate how their sustainability initiatives drive improved shareholder returns and access to investor capital.
As these five trends transform the way we deliver health sciences and wellness, companies must understand that Future (Health) Value lies in unlocking the power of data to create Health Experience.

Related articles
Summary
COVID-19 has accelerated the broader digital transformation of health care delivery, highlighting the gap between companies’ current capabilities and what is required for future growth.
Demand from the patient-consumer has accelerated the acceptance and adoption of new technologies and the data that fuels them. This data-driven transformation will enable personalization at unprecedented levels and disrupt every area of the established value chain across the health sciences and wellness sector.


